
Today, we attempt to tackle the giant topic of pain management in our four-legged family members. In the grand scheme of veterinary medicine, this is actually a fairly recent concept and there is still a lot of research and work to be done. There are unfortunately also a lot of misconceptions about pain in animals that veterinarians are working hard to overcome. We want to help you understand what pain looks like in our dogs and cats, why it is so important to try to control it, and the integral role you play, as the pet parent, in making this all happen.
We also approach pain in our pets from a personal place of great understanding. We know first-hand of the struggles our pet parents face when it comes to recognizing pain in their own pets. While we can pinpoint with great accuracy the cause of pain in so many of our patients every day, we missed it in our own dog for a period of time. Often these changes happen so gradually they are really tough to detect. Our pets (cats in particular) are masters at hiding pain and illness. The day they come to you and act like they are in pain, they most likely have been suffering in silence for quite some time. Finally, we know it is difficult for pet parents to see pain in their own pets because of what it might mean. To recognize that your pet is in pain is to admit there might be something wrong, and that saddens and terrifies us all at once.
However, the important thing to remember is that you are not alone in all of this. You do not have to know what is wrong, you just have to know that something is not right. Once we were able to see that our dog was just not quite herself, we reached out to colleagues to help us with the rest. We are so thankful we trusted our guts and sought out help, because it made a world of difference in how our dog felt within just a few days. Hopefully this information will help you do the same for your furry friend if you are ever in the same boat.
What are the signs of pain?
First, let’s investigate what pain may look like in a dog or cat. Some of these changes may come on all at once or happen gradually over time, but recognizing them can get your pet the care they need sooner rather than later.
-
Limping:
This one may seem fairly obvious as a sign of pain, but it is surprising to our team how many pet parents will mention that their dog or cat is limping, but does not seem to be in pain. We notice that this happens more with chronic limping, but has also been heard even when there was history of recent trauma. We think it is because pet parents expect their pet to cry out or whimper when they are in pain. However, it is incredibly rare for a dog or cat to actually cry in pain. The vast majority of the time, the limping is the ONLY sign you will get that your pet is in pain. Think about what causes you to limp. Often we are changing our body’s natural movement to prevent putting weight on one leg. This is exactly what our pets are doing too.
-
Hiding:
This behavior is especially true in cats, but can also happen with dogs. When animals are in pain, they may choose to isolate themselves. This may mean they spend the majority of their time in a different room than the rest of the family. In extreme cases, this can even mean they hide behind furniture, under the bed or in a closet. However, more often than not, hiding/isolation is much more subtle. This may mean this pet is in the same room as the other pets or family members, but positions himself along the margins of the room or higher up on the furniture. They may also go out to the yard and purposefully stay away from the activity. They may even choose to separate themselves from younger members of the family who are not as gentle and may exacerbate pain with rough play or interactions. While this can sometimes be a behavioral strategy, it may just be a protective move because of the underlying chronic pain a pet is experiencing.
-
Change in Daily Activities:

This is a particularly subtle indication of pain and, is frequently overlooked because of how slowly this change occurs. This category can represent a lot of activities, but here are a few common ones to consider:
-Does your pet no longer greet you at the door, or when you get up in the morning?
-Has your pet stopped playing with their favorite toys, or perhaps plays just slightly less frequently or with less gusto?
-Does your pet get up to get water less frequently than before?
-Did they stop spending time on the bed, couch, cat tree, or what ever other place used to be their favorite spot?
-Does your cat take two jumps instead of 1 to get to higher furniture? Do they hesitate before making the jump?
-Does your dog get less excited for walks or walk less distance?
-Do they no longer enjoy being petted in certain spots?
-Does your dog or cat no longer go up or down the stairs?
-
Decreased Appetite/Picky Appetite:
Please keep in mind that this is one key area where every pet is different. There are some animals that experience pain and almost immediately stop eating, while there are others who could be walking around on a broken leg, but would still happily gulp down food. So please do not assume that just because a dog or cat is still eating that they must not be in pain.
It has been shown that pain can cause secondary nausea and stomach upset. Some pets may experience this side effect of pain to a greater extent than others, and often those pets will show a decrease in appetite or become pickier about what they choose to eat.
In addition to experiencing nausea, there are some forms of pain that will make it more difficult to eat. For example, dental pain or neck/back pain can make chewing or bending over to pick up food much more challenging.
-
Slowness/Stiffness Getting Up or Difficulty Walking On Slippery Floors:
One question you may hear our veterinarians ask during annual examinations is “how well is your pet getting around?” Unfortunately, while many pet parents may recognize that their dog or cat is slowing down or struggling, they will also justify this behavior with their pet getting older. Of course, some diseases like arthritis are more common with older pets, but it is the pain associated with these diseases that is causing your pet to slow down. One of the most common signs of this type of pain is being slow to rise or not wanting to jump on furniture. You may also see your pet not want to jump in the car. It is also important to remember that while getting older may be inevitable, pain is not. We have come a long way in medicine with managing pain, and in some cases, can make your dog or cat behave like a puppy or kitten again with a few recommendations.
-
Urinary and/or Fecal Accidents:
There is a laundry list of reasons why a pet might have urinary or fecal accidents in the house. In a previously house-trained pet, the vast majority of these are medical reasons, with one of them being pain. This pain could be coming from arthritis, but it may also be coming from disc disease, a urinary tract infection, bladder stones, anal gland abscesses or any other potential source of pain an animal may have. If a pet feels so uncomfortable getting up to go outside or experiences pain during urination or defecation, they may choose to perform those things inside. This is also true of cats who experience pain while in the litter box. Sometimes they will associate this pain with the litter box itself and choose to urinate or defecate in other areas of the house.
One heart-breaking difference between owner’s perception of dogs and cats is noted in this sign of pain. Most dog owners quickly recognize that inappropriate urination or defecation may be medically related and bring their pet to a veterinarian in the early phase. However, there is a bit of a misconception regarding inappropriate urination with cats, in that it is frequently viewed as a vindictive or behavioral issue. However, cats can have many of the exact same medical issues that cause them to urinate in the house. Even behavioral factors such as stress can cause a serious physical condition called cystitis (inflammation in the bladder) that causes pain, which is actually what leads to the inappropriate urination. This chronic pain can then keep the inappropriate urination going long after the initial stress factor has disappeared.
-
Standing or Sitting in Hunched Positions:
Again, this may be one of those signs that is much more difficult to notice than some of the more obvious ones, but it can be equally as important. With back pain or abdominal pain, it is really common for dogs to lie down or stand in a slightly hunched position. They may also seem restless and unwilling to settle (mostly because they cannot find a position in which they are comfortable).
Cats will also stay in a hunched position particularly for abdominal pain. Often, they are lying down with their legs tucked in close to them. They may couple this with the isolation or hiding behavior. They will be very hesitant to stretch out, jump or even walk.
-
Overgrooming or Licking a Particular Spot:
In addition to things like allergies, infection or fleas, a pet may also overgroom if they are experiencing pain in one particular area. It is their attempt at alleviating the discomfort, often coming from a deeper part of the body like the abdomen or a joint. On the other end of the spectrum, cats that suddenly stop grooming may also be experiencing pain. Before long, their haircoat will become unkempt and sometimes even matted. Sorting through pain as the underling cause may take a little investigative work, but is well worth the pursuit.
-
Weight Loss/Muscle Loss:
Muscle loss is quite common with chronic pain associated with arthritis. Usually a pet will choose to walk or exercise less. If they have one area of the body that has more significant arthritis than other areas, they may choose to shift weight. For example, a dog with hip dysplasia, who is experiencing pain in their back end will preferentially put more weight on their front legs. This subtle change in gait may be really difficult to notice. However, as weeks or months go by, the muscles in the back legs and along the back of the spine may start to shrink in size from disuse. As this happens, a pet becomes weaker and weaker making the simple act of standing difficult. Once the muscle loss has occurred, it is much more difficult to correct, than if the pain is addressed prior to muscle loss occurring.

-
Aggression:
We all have lost our temper or been more irritable from time to time when we are not feeling well. The same changes in behavior can happen in our pets. It is frustrating, confusing and frankly miserable to be in pain. Afraid that certain interactions will lead to heightened pain, pets may become protective of themselves and growl, hiss, snap or strike instinctually. If there is a sudden change in behavior in an otherwise mild-mannered pet, pain or illness should be a top concern.
I Think My Pet Might Be in Pain. What do I do?
- Do Not Wait: If there is only one thing to remember from this entire blog, this is it-if you think there is any chance your pet is in pain, have them examined by your veterinarian. Do not wait. Not only is there potential for your pet to suffer if treatment is delayed, but some acute causes of pain like pancreatitis, foreign bodies, urinary obstructions or disc disease can cause life-threatening or irreversible changes very quickly.
 However, chronic pain should be taken just as seriously. Chronic dental pain is often associated with infection. That same oral infection can cause permanent damage to the heart, kidneys, liver or lungs. Even arthritis, which tends to come on slowly and does not seem to pose a serious threat, often leads to muscle loss and weakness, which can make it difficult for a pet to stand. The inability to stand is one of the most common reasons pet parents elect euthanasia in large dogs. However, when detected early, and the pain managed, this muscle loss can be slowed or even stopped.
However, chronic pain should be taken just as seriously. Chronic dental pain is often associated with infection. That same oral infection can cause permanent damage to the heart, kidneys, liver or lungs. Even arthritis, which tends to come on slowly and does not seem to pose a serious threat, often leads to muscle loss and weakness, which can make it difficult for a pet to stand. The inability to stand is one of the most common reasons pet parents elect euthanasia in large dogs. However, when detected early, and the pain managed, this muscle loss can be slowed or even stopped.
2. Diagnostics are Important: A thorough exam with a veterinarian is going to be a critical first step in assessing your pet’s pain. In some cases, a physical exam alone can diagnose the cause of your pet’s pain. However, there may be a lot of times when the exam isolates the pain to one region (abdomen, back, mouth), but additional tests are absolutely necessary to get answers and start treatment.
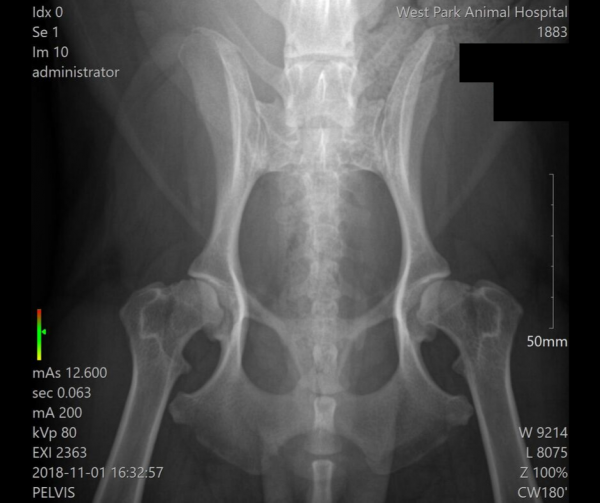
For example, your veterinarian may be able to tell you with great confidence that your cat has abdominal pain. They may even be able to tell you based on your cat’s response that pain is coming from the top (cranial) part of the abdomen. However, it’s the x-rays/ultrasound and bloodwork that may help them know if this pain is from pancreatitis, a foreign body, gall stones or a kidney infection.
Even things that might seem fairly obvious can be horribly misdiagnosed without running the right tests. On more than one occasion, we have had a senior dog come to us with what was originally thought to be arthritis. However, upon running some screening tests for tick transmitted diseases, we found these dogs actually had joint pain at least in part because of their infection.
3. Treat the Underlying Cause: This may seem like a very simple concept, but there are a lot of diseases where it gets grossly overlooked. If a dog has a foreign body in its intestines, most pet parents want to quickly have it removed. However, in the case of feline cystitis (bladder inflammation), pain management can make a cat feel better fast, but does not always get to the root of the problem. Is there a stress factor that needs to be addressed? Would some changes to the environment help? Is this cat forming small crystals in its urine that are causing inflammation? The path to treatment may not be quite as clear-cut, but is equally as important to work through.
Let’s Get Them Feeling Better!
Regardless of the cause, one of the top goals for our veterinarians is to control pain. We NEVER want our patients to suffer, which means we recommend pain management with whatever treatment route we pursue. If we think your pet is experiencing significant pain, we may even recommend managing it before putting them through the process of taking x-rays or drawing blood. Once we know we have started to control pain, we absolutely need to pinpoint the source of it and start treating the underlying cause. The more we understand why your pet is experiencing pain, the better we are able to control it, and we have many tools to help us do just that!
- Medications: There are a wide variety of drug classes to help control pain. When the pain is acute or first being diagnosed, we utilize these medications to help get our four-legged friends feeling better fast. One very important thing to keep in mind here is that our dogs and cats are not small humans. They may take similar drugs like opiates and NSAIDs, but the exact types of drugs, how they are metabolized and the doses vary greatly from humans, and even between cats and dogs. One glaring example of this is the use of human medications like Tylenol in cats causing life-threatening liver failure. It is always best to consult your veterinarian before giving your pet any pain medication.
- Diet and Weight Loss: It is shocking how much weight loss and diet therapy can make a huge difference in a pet’s quality of life. With joint disease and disc disease in particular, weight loss can alleviate much of the pressure being placed on these areas and dramatically reduce pain over time. Excessive fat has also been linked to some inflammatory processes in the body, so weight loss can also help reduce some inflammation. This leads to better pain control. In some of our patients, weight loss alone has allowed them to come off of medical pain management and still be quite comfortable.
There are specific prescription diets available to help manage inflammation associated with joint disease such as Hills j/d or Purina JM. Also, in cases of cats with cystitis, diet therapy may reduce crystal formation or even help with the stress component involved.
- Physical Therapy/Laser/Acupuncture: The value of physical/rehabilitation therapy cannot be underestimated in the control of pain especially when it comes to diseases affecting the muscles, skeleton and nerves. Physical therapy helps maintain strength and flexibility, which creates less risk of injury to the affected areas. Low level laser and acupuncture may also be helpful in reducing inflammation and managing pain response to certain diseases.
- Supplements: This is a category of pain management that is unregulated. While there are some supplements, such as fish oils or glucosamine, that have some science to support their use, there are a lot of supplements on the market that make grand, but unfounded claims. Please be weary of what you may read on marketing labels, as their whole purpose is to sell you this product. Even some supplements that have some data to support their use in people may not be safe or effective in dogs or cats. As we have previously mentioned, dogs and cats are definitely not small people. The types of drugs and sometimes the doses they can tolerate can vary widely. It is also important to note that these products are not FDA regulated, so consult with your veterinarian about trusted brands and dosing.
- Environmental Changes: While small adjustments in the home may not control pain or treat the disease, they may make a world of difference in your pet’s quality of life. For example, if your cat is really struggling to jump on the counter for their food, we should try to find a more easily accessible location for feeding. Adding ramps or stairs around the home allows your senior pet to still do some of the things they love without having to jump. Even simple changes like adding extra litter boxes or water bowls makes the necessary resources readily available and alleviates any stress your pet may be feeling about getting to what they need.
Summary
The signs of pain in pets are often subtle and can go unnoticed if we don’t pay special attention to look for them. There are many options for treating or even preventing pain, but starting early is definitely best. If you think your pet is experiencing pain, our veterinarians are here to help. They want your pet to be as pain-free and comfortable as possible, no matter their life stage. To set up an appointment to speak with one of them, give us at a call at (813) 749-6863 or book online via our website.







Leave A Comment